To comment or receive more such wisdom, please register on www.gyanalogy.com/login
For ages, the common and faulty understanding has been to observe people who have mental illness as “lunatics,” “dangerous,” and “violent people” who need to be secluded from society.
The sustainable development goals were built on the principle of leaving no one behind. The current theme of World Mental health day aims at Mental Health for All. The World Federation of Mental Health states that mental health is the most urgent concern and calls for action, which can no longer be ignored. Dr. Daniels, the President, quoted, “Mental health is an investment and not an expense and should be prioritized to avert a further catastrophe.”
On this premise, the world placed its asylums in the peripheries. This sad yet unfortunate belief is further perpetuated by how books and movies portray mental illness, treatment, and mental health professionals. In today’s world striving for ‘Human Rights,’ where India is one of the signatories of the United Nations Convention on Rights for People with Disabilities (UNCRPD), it is a fundamental and well-deserved ‘right’ of a mentally ill individual to be included in the community for his/her living. This social inclusion fosters improvement in any psychiatric disorder, as much as medicines or counselling. Where a ‘greater investment’ can achieve this, however, stands the test of time!
The treatment gap is 50 percent in the high-income countries and 85 percent in lower and middle-income countries. The roadblocks have been fragile health systems, lack of trained healthcare professionals, low clinician to client ratio, increased stigma, misinformation, resistance to change, poor collaboration between media, administration & healthcare professionals, and societal apathy. These roadblocks are compounded now by the current crisis, thanks to COVID-19. Another valid point that the outbreak has brought to light is the disparity in mental health needs, which is highly tailored and individualized. This disparity especially applies to a socio-culturally diverse and populous country like India, where the ‘connotations and understanding’ of mental health itself is exceptionally heterogeneous. This ‘disparity’ needs a separate discussion altogether. Let’s just say: the approach to urban loneliness and health anxiety of the affluent societies will be quite different as compared to dealing with the existential crisis of each day, as faced by the lesser privileged classes (homeless, migrants, etc.), who form the bulk of the populace.
Mental Wellbeing vs. Disorder: The ‘Grey Lines’ of Divide
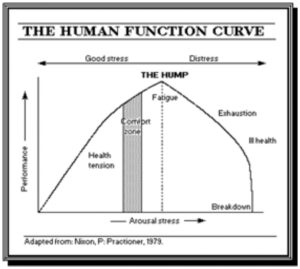
(The American Institute of Stress, 2011; with permission)
While explaining stress, Hans Seyle stated that it is the body’s non-specific response to any demand for change and concluded that it could be both the cause and result. Two variables affect the stress response in an individual, namely the performance expectation and arousal stress. Stress is ‘good stress’ till the time it exists and maintains in the comfort zone, but the moment the zone is breached, “The Hump” is created, resulting in the fall in the curve with the stages of fatigue, exhaustion, ill-health, and eventually resulting in a breakdown. Mental well-being is the ability of an individual to adapt and maintain good stress, thereby allowing for good bio-psycho-social functioning. At the same time, the breach makes the person maladapt or difficult to function independently. The inability interferes with physical, social, and psychological functioning resulting in increased dependence on the family members, “The Hump” is created, resulting in psychological and psycho-social concerns, thereby leading to disorder.
Present Times: The Enhanced Need
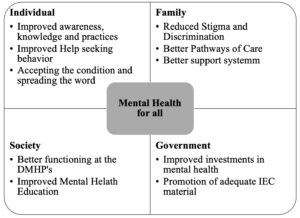
The current pandemic has increased the focus on mental health, thereby stating the importance of improving the care and establishing the continuum of care. Hence focus remains to develop the plan of management to ensure mental health for all. One needs to have a strategy based on the individual, family, and societal levels to provide greater access. This ‘renewed importance’ needs to outlast the pandemic and be the usual norm: to strive to stay mentally healthy and promote psychological health!

Epilogue
As commonly said, “Mental Health is a Process, Not a Destination! It doesn’t matter where life takes you, but how you are driving”.
Psychiatric problems are NOT ‘myths’! They are ‘real’ diseases that need treatment, can be treated, and, most importantly, prevented. The common faulty analogy of depression confused with “feeling sad” is equally harmful as equating ‘runny nose’ with pneumonia. “Not feeling mentally well” is an equally important reason to seek professional help and if associated with the ‘DANGER signs’ (loss of sleep, appetite, weight loss, severe sadness, guilt, difficulty in personal or professional life, death wishes, etc.), need URGENT PROFESSIONAL HELP. Hanging out with friends, drinking or smoking, or watching a good movie might be temporary relief but not pragmatic SOLUTIONS.
This Mental Health Day, let’s think beyond a ‘day,’ plan beyond the ‘pandemic,’ and look beyond ourselves: for a ‘greater emotional investment’ in mental health promotion and ending stigma, to serve a greater good!

Dr Debanjan Banerjee is a Psychiatrist, National Institute of Mental Health and Neurosciences (NIMHANS), Bengaluru and Life Fellow, World Psychiatric Association. He is M.D. Psychiatry (NIMHANS), FIPS, FIASP, FIAGMH, D.M. Geriatric Psychiatry Senior Resident, NIMHANS, Associate Editor, Frontiers in Psychiatry: Aging Psychiatry, Assistant Editor, Journal of Psychosexual Health (SAGE), Assistant Editor, Journal of MHE, NIMHANS

Ms Vasundharaa S Nair is a Psychiatric Social Work PhD. Fellow, NIMHANS, Bengaluru
The views, thoughts, and opinions expressed in the article belong solely to the author.
To comment or receive more such wisdom, please register on www.gyanalogy.com/login




